According to the RACGP, (Royal Australian College of General Practitioners).
Australia ranks first among OECD countries for equity and healthcare outcomes, and holds third place for overall healthcare performance, behind Norway and the Netherlands.
In terms of access, Australian patients reported having high levels of access to face-to face care when needed, but lowest levels of same-day responses to questions by email or phone. Dr Wright notes, however, that this has potentially changed since the introduction of telehealth after the report’s survey was completed.
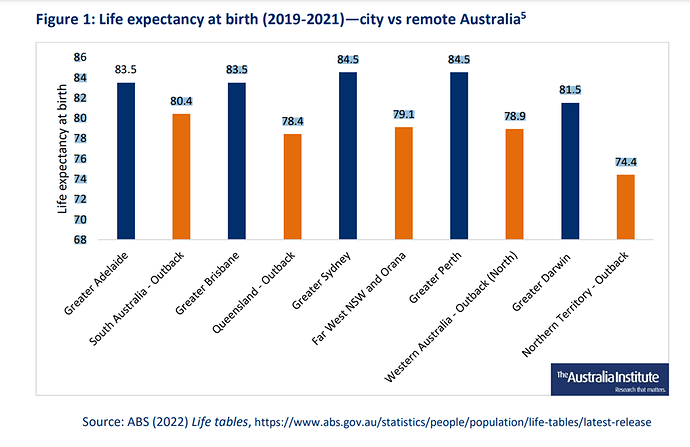
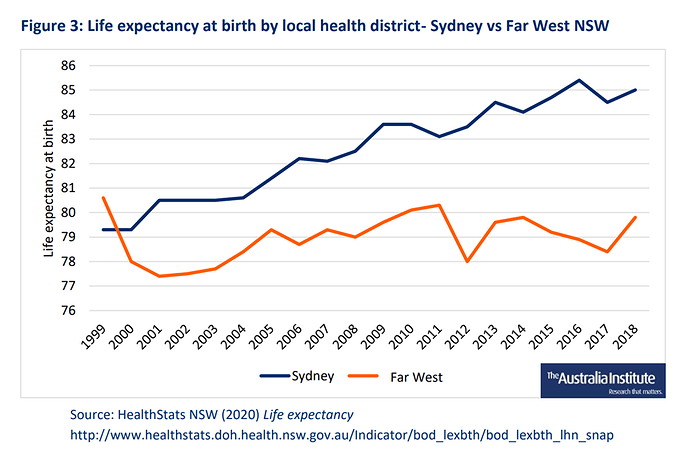
The majority of Australians live in our 6 largest cities or nearby, and that’s where the majority of the medical resources are. It’s easy to overlook how it is for a minority living elsewhere?
What works well in rural and regional Australia for health care, and what can be be better or differently to improve the outcomes?
Edit: note Australia has approx 31,000 GP’s, or one for every 850 of us.
‘Medical doctors and specialists in Australia | Australian Government Department of Health and Aged Care
Opening post inspired by the following.